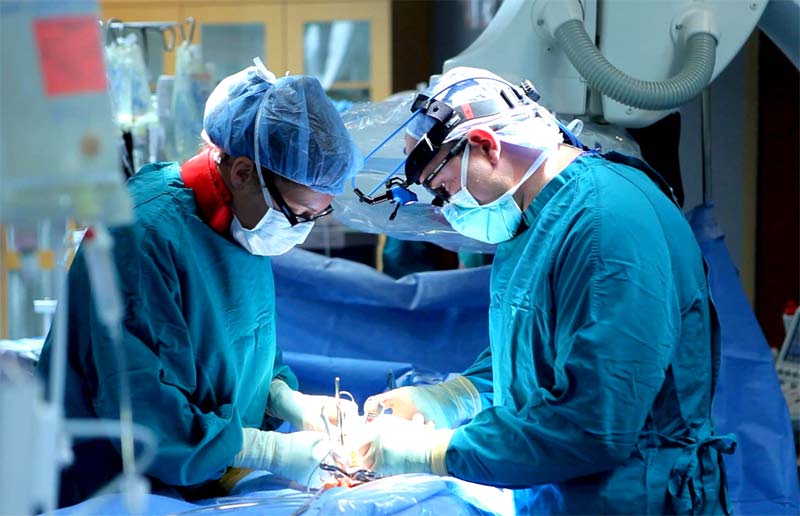
Thyroid surgery is a possible treatment for individuals who suffer from thyroid conditions such as hyperthyroidism or thyroid cancer. Doctors will usually attempt to treat a thyroid condition using medication first.
If non-surgical methods do not work to alleviate or manage symptoms effectively, thyroid surgery is often the next line of procedure. Through this type of surgery, doctors are able to eliminate the problem for good since the operation actually removes the source of the problem – the thyroid gland.
The thyroid gland is located in the neck. It is a small gland that wraps around the trachea or windpipe. The thyroid produces thyroid hormones which help the body use energy, stay warm and keep the brain, heart, muscles, and other organs working normally. Thyroid operations may be needed for patients who have a range of thyroid disease, including both cancerous and benign (non-cancerous) thyroid nodules, large thyroid glands (goitre), and overactive thyroid glands (hyperthyroid).
The most common reason patients are referred for thyroid surgery is after an evaluation for a thyroid nodule. Surgery is also an option for the treatment of hyperthyroidism and for any goitre that may be causing symptoms. Surgery is definitely indicated for a diagnosis of thyroid cancer or the possibility of thyroid cancer. In the absence of a possibility of thyroid cancer, there may be non-surgical options of therapy. You should discuss other options for therapy with your doctor.
Thyroid surgery may be needed when the thyroid is:
- Overactive (hyperthyroidism or thyrotoxicosis) and medical management is unsuccessful
- Enlarged or nodular
- Producing pressure symptoms causing breathing difficulties, choking, or the sensation of lump in the throat
- Cancerous or is suspected of being cancerous
- Enlarged and unsightly
- Growing into the chest
About Thyroid Surgery
Hemithyroidectomy
 Hemithyoidectomy surgery removes of one of the thyroid lobes. Hemithyroidectomy is the minimum surgical procedure for adequate treatment of a solitary thyroid nodule. This is a safe operation with a minimal risk of damaging either the parathyroids or the laryngeal nerves.
Hemithyoidectomy surgery removes of one of the thyroid lobes. Hemithyroidectomy is the minimum surgical procedure for adequate treatment of a solitary thyroid nodule. This is a safe operation with a minimal risk of damaging either the parathyroids or the laryngeal nerves.
There are several indications for hemithyoidectomy surgery including thyroid nodules and suspected thyroid cancer, compression symptoms, hyperthyroidism due to a solitary hyperfunctioning thyroid nodule or cosmetic reasons such as an unsightly lump in the front of the neck.
Minimal Access Thyroidectomy
 Minimal Access Thyroid surgical techniques allow removal of part of the thyroid gland through a mini-incision approach. This approach may be used for patients who require a hemithyroidectomy, thyroid isthmusectomy or local thyroid nodule excision.
Minimal Access Thyroid surgical techniques allow removal of part of the thyroid gland through a mini-incision approach. This approach may be used for patients who require a hemithyroidectomy, thyroid isthmusectomy or local thyroid nodule excision.
Minimal access thyroid surgery is a safe and feasible alternative to open thyroid surgery in selected cases. Major advantages of minimal access techniques include reduced tissue trauma, shorter hospital stay, better cosmetic results, minimal postoperative pain, reduced cost of healthcare and, better patient comfort.
Total Thyroidectomy
 Total thyroidectomy involves removing all or nearly all of the thyroid gland. It may be done for benign thyroid conditions that affect both thyroid lobes, such as large goiter or Graves’ disease, or it may be done for cancer.
Total thyroidectomy involves removing all or nearly all of the thyroid gland. It may be done for benign thyroid conditions that affect both thyroid lobes, such as large goiter or Graves’ disease, or it may be done for cancer.
A near-total thyroidectomy means that the surgeon decided to leave a very small amount of benign thyroid tissue behind. Total thyroidectomy is routinely performed under general anaesthesia. The in-hospital length of stay after total thyroidectomy is usually one night.
Thyroid Surgery Recovery
Thyroid surgery recovery
 After your thyroid surgery, you will be taken to the recovery room. It is normal to feel some pain in your neck after a thyroid procedure.
After your thyroid surgery, you will be taken to the recovery room. It is normal to feel some pain in your neck after a thyroid procedure.
Your throat may also be sore, and it may hurt to talk and swallow. This is normal immediately following the procedure. In most cases, you will stay in the hospital for the first night of your recovery to be monitored for any complications. Most patients are able to return home within 24 hours after the procedure. Before your discharge, you will be given instructions on how to care for your surgical incision and when to see your thyroid surgeon.
Care after thyroid surgery
 Once you have recovered from the effects of thyroid surgery, you usually will be able to doing anything that you could do prior to surgery. If needed your thyroid replacement may begin immediately after your surgery or it may be started several weeks later, depending upon the condition that made the surgery necessary. Once hormone replacement is started, it will need to be monitored to prevent the symptoms of hyper or hypothyroidism.
Once you have recovered from the effects of thyroid surgery, you usually will be able to doing anything that you could do prior to surgery. If needed your thyroid replacement may begin immediately after your surgery or it may be started several weeks later, depending upon the condition that made the surgery necessary. Once hormone replacement is started, it will need to be monitored to prevent the symptoms of hyper or hypothyroidism.
The level of calcium and vitamin D in your blood may also be monitored. In some cases, a daily supplement will be necessary. This is especially true if the parathyroid glands were involved in the procedure.
The possible risks from thyroid surgery include bleeding that can cause acute breathing difficulty, injury to the recurrent laryngeal nerve that can cause hoarseness, and damage to the parathyroid glands that control calcium levels in the body, causing hypoparathyroidism and hypocalcemia. The overall risk of complications should be less than 2% with an experienced surgeon.
Frequently Asked Questions
Thyroid surgery FAQs
 Surgery will be recommended if the thyroid disease cannot be adequately treated medically. Depending on the specific condition, the extent of thyroid surgery will vary.
Surgery will be recommended if the thyroid disease cannot be adequately treated medically. Depending on the specific condition, the extent of thyroid surgery will vary.
Thyroid surgery procedures may remove only one lobe of the thyroid, or half of the gland (this procedure is called a thyroid lobectomy or hemithyroidectomy – to remove the entire thyroid, called a total thyroidectomy.
Thyroid surgery may be performed through a standard neck incision or by a mini-incision (minimal access thyroid surgery) depending on the underlying thyroid condition. Sometimes the extent of surgery must be determined during surgery when the features of the thyroid disease can be seen directly.
If you have questions about thyroid surgery, contact your local doctor who will arrange for you to see a thyroid surgeon.